2 Week Orthopaedic Review
Phase 1 Goals:
- Full extension to 90° flexion
- Wound healed
- Minimal swelling
- Normal Gait
Your experience and care before your knee surgery, during and post surgery is at the forefront of Chan Jeer Orthopaedics activities.
Chan Jeer will explain in detail before your surgery what the recovery and aftercare will be. General health, your profession and severity of knee issue will impact the length of your recovery and the exercises needed.
One of our rehabilitation methods is ACL Reconstruction Rehabilitation. You can learn more about ACL Reconstruction Rehabilitation here with one of Chan Jeer’s case studies.
The guidelines described below are not a strict protocol and can vary for each individual.
PRE-OP
Rehabilitation begins before surgery in the pre-operative phase to ensure that you and your knee are ready for the operation.
Day of Operation
Day 1 and 2 Post-Op
Aims on Discharge
Your rehabilitation within the physiotherapy department will commence approximately two weeks after discharge and once the clips, (used to hold wound together), have been removed. The rehabilitation programme provided within the Physiotherapy department aims to safely progress you through the milestones. You will be shown the exercises which will most effectively allow you to achieve these milestones. Most of the exercises require very little equipment and have been developed to allow you to continue your rehabilitation at home. You will be expected to continue the exercises taught to you by the physiotherapist until you are seen in the outpatient physiotherapy department for further rehabilitation. Pain and swelling should be your guide with regards to the amount of exercise you can undertake.
You will have a Consultants review 2 weeks post surgery where your clips will be removed and an x-ray taken on arrival.
Precaution – for the first 6 weeks following your orthopaedic surgery do not:
The exercise programme consists of five main phases namely:
It is advisable to perform the exercises described below on a daily basis and not only within the physiotherapy department.
Aim:
The aim of this phase is to regain movement in the knee, allow swelling to settle and to encourage a normal gait pattern.
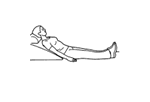
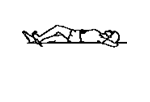

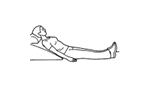








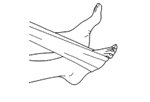

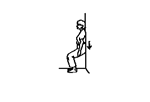



Aim:
The aim of this phase is to introduce proprioceptive exercises and gradually improve strength and endurance. By the end of 6 weeks your knee should feel normal in activities of daily living.
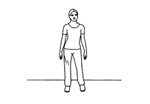
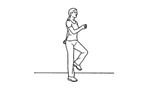
Week 2 exercises including:
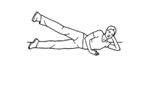

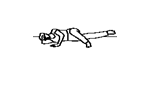

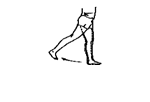

Aim:
At this stage the hamstring graft will have become solidly fixated within the femur and tibial tunnels. This allows for more vigorous strength training to commence. There are no specific precautions at this stage, but it is important to avoid too rapid progress as there is a risk of developing complications associated with overloading. The physiotherapist will monitor your strength and control, and progress as appropriate.
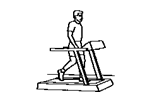

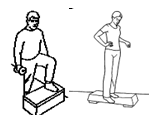


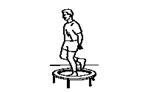


Aim:
The aim of this phase is to introduce pivoting and cutting exercises which play an important role in returning to sporting activities. This stage includes agility and power training starting slowly and progressing to moderate speeds.
If your occupation involves manual work it should be possible at this stage depending on the requirements of the occupation.







Aim:
This phase is aimed at progressing training to create a foundation for the return to full sporting activity.
It is not recommended to return to full contact sport until the functional and strength outcomes are measured at greater than 85% of the normal side. To build up the confidence and regain pre-injury level of skill and performance is variable and can take 3 to 4 months of training and playing. It is recommended that you progress your training within your specific sporting environment.
Progress is best achieved in conjunction with a general fitness programme and full contact is best avoided until you are able to tolerate full training sessions and are confident with your fitness and endurance.
No Contact Sports Until After 9 Months